Understanding Psoriasis: Causes, Symptoms, and Treatment Options
By:

Apex Hospitals
22-07-2023 5 Min Read
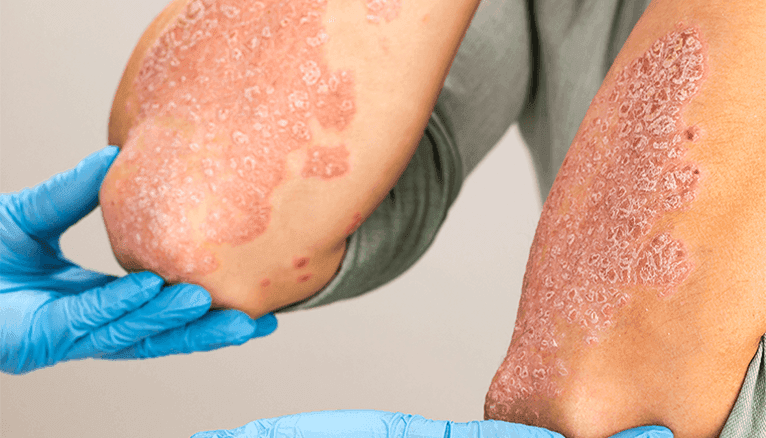
Psoriasis is a chronic autoimmune disease that affects the skin, causing red, itchy, and scaly patches to develop. It is a common condition, affecting approximately 2-3% of the global population. Living with psoriasis can be challenging, both physically and emotionally.
What is Psoriasis?
Psoriasis is a non-contagious skin condition characterized by rapidly producing skin cells. Skin cells mature and shed in a healthy individual every 28 to 30 days. However, this process is significantly accelerated in people with psoriasis, with skin cells growing and shedding within 3 to 4 days. As a result, the accumulation of excess skin cells leads to red, scaly patches on the skin's surface.
Inflammation and redness are relatively prevalent around the scales. Psoriatic scales are often whitish-silver and appear in dense, red patches. They can, however, appear purplish, dark brown with grey scales on darker skin tones. These patches will occasionally shatter and bleed.
Scales commonly form on joints such as the elbows and knees. They can, however, appear anywhere on your body, including the following:
- hands
- feet
- neck
- scalp
- face
Less prevalent forms of psoriasis affect:
- nails
- mouth
- the region around the genitals
Understanding the Causes of Psoriasis
While the exact cause of psoriasis remains unknown, it is believed to result from a combination of genetic and environmental factors. Research suggests that specific genes may play a role in developing psoriasis, as it tends to run in families. Additionally, environmental triggers, such as infections, stress, and certain medications, can exacerbate the condition in genetically predisposed individuals.
The Different Types of Psoriasis
Psoriasis can manifest in several different forms, each with its unique characteristics. There are five types of psoriasis.
- Plaque Psoriasis is the most common type of psoriasis, accounting for approximately 80% of all psoriasis cases. It causes red, inflamed spots on light skin tones and purple, greyish, or darker brown areas on darker skin tones, making it more difficult to identify in people of colour. These patches are sometimes coated with whitish-silver scales or plaques and are frequently more severe on the skin of colour. The elbows, knees, and scalp are common sites for these plaques.
- Inverse Psoriasis: Inverse psoriasis produces bright red, shiny, irritated skin. Patches of inverse psoriasis appear behind your armpits or breasts, in your groin, or around genital skin folds.
- Pustular Psoriasis: Adults are more likely to develop pustular psoriasis. Depending on skin tone, it causes white, pus-filled blisters and large regions of red or violet-inflamed skin. It can appear as a more intense violet tint on darker skin tones. Pustular psoriasis is commonly found in smaller body parts, such as the hands or feet, but it can be widespread.
- Erythrodermic psoriasis is a severe and highly uncommon form of psoriasis. This shape frequently covers significant areas of your body at once. The skin seems to be sunburned. Scales that form frequently slough off in substantial portions or sheets. With this type of psoriasis, you may develop a fever or become pretty unwell. This type of infection can be fatal, so make an appointment with a healthcare expert immediately.
- Guttate Psoriasis: Guttate psoriasis is more frequent in children. This kind of psoriasis causes small pink or violet patches. Guttate psoriasis most commonly affects the torso, arms, and legs. These areas are rarely dense or elevated, as with plaque psoriasis
Understanding the Causes of Psoriasis
While the exact psoriasis causes remain unknown, it is believed to result from a combination of genetic and immune systems.
Genetics:
Some people inherit genes that increase their risk of developing psoriasis. If you have an immediate family member with a skin condition, you are more likely to have it yourself.
Immune System:
Psoriasis is an autoimmune disease. Autoimmune diseases are caused by your body attacking itself. White blood cells, known as T cells, wrongly attack your skin cells in the case of psoriasis. This produces the plaques most frequently associated with psoriasis. Attacks on skin cells also result in red, inflammatory regions of the skin.
Common Triggers for Psoriasis Flare-ups
External “triggers” may start a new bout of psoriasis. These triggers are not the same for everyone. They may also change over time for you.
The most common triggers for psoriasis include:
- Stress: A flare-up may be triggered by very high pressure. You can lessen and possibly prevent outbreaks if you learn to reduce and manage your stress.
- Alcohol: Psoriasis flare-ups can be exacerbated by alcohol use disorder. Psoriasis outbreaks may be more common if you drink heavily. Consider limiting or eliminating alcohol use for reasons other than your skin.
- Injury: A flare-up might be caused by an accident, wound, or scrape. Injections, immunizations, and sunburns can potentially cause a fresh outbreak
Signs and Symptoms
Psoriasis symptoms can vary from person to person. The most common symptoms of psoriasis include:
- Patches of elevated, irritated skin that appear red on light skin and brown or purple on dark skin
- whitish-silver scales or plaques on the red patches or grey scales on the purple and brown patches
- skin that is dry and may crack and bleed
- Soreness around patches
- Thick and pitted nails
- itching and burning sensations around the patches
- painful as well as swollen joints.
The majority of persons with psoriasis experience "cycles" of symptoms. The illness might cause severe symptoms for a few days or weeks, then clear up and become nearly unnoticed. The problem may then flare up again in a few weeks or if aggravated by a common psoriasis trigger. Psoriasis symptoms might sometimes entirely disappear.
Is Psoriasis contagious?
One common misconception about psoriasis is that it is contagious. However, psoriasis is not infectious and cannot be transmitted through direct contact or sharing personal items. It is an autoimmune disease that results from an overactive immune response rather than a bacterial or viral infection.
The Connection between Psoriasis and Arthritis
In addition to affecting the skin, psoriasis can also have an impact on the joints, leading to a condition known as psoriatic arthritis. Approximately 30% of individuals with psoriasis develop psoriatic arthritis, which can cause joint pain, stiffness, and swelling. Psoriatic arthritis can affect any joint, including the fingers, toes, knees, and spine.
Individuals with psoriasis must know the potential risk of developing psoriatic arthritis. Early detection and treatment of psoriatic arthritis can help manage symptoms and prevent further joint damage.
Diagnosis of Psoriasis
To diagnose psoriasis, two tests might be necessary.
- Physical examination: A simple physical exam is enough for most clinicians to make a diagnosis. Psoriasis symptoms are usually evident and easy to identify from those caused by other illnesses.
- Biopsy: If your symptoms are unclear or your doctor wants to confirm a suspected diagnosis, a small skin sample may be taken. This is referred to as a biopsy. The skin biopsy will then be sent to a lab for investigation and inspected under a microscope. The exam can determine the type of psoriasis you have. It can help rule out other diseases or infections.
Psoriasis Treatment Options
In addition to self-care strategies, various treatment options are available for individuals with psoriasis. Treatment choice depends on the severity of the condition and the individual's response to previous treatment attempts.
- Topical treatments, such as corticosteroids, vitamin D analogues, and retinoids, are often prescribed for mild to moderate psoriasis. These medications are applied directly to the affected skin and work by reducing inflammation and slowing down the growth of skin cells.
- For more severe cases, systemic treatments may be recommended. These include oral medications or biological therapies, which target specific components of the immune system involved in psoriasis.
- Phototherapy, or light therapy, is another treatment option that uses ultraviolet light to slow down the production of skin cells and reduce inflammation.
How to Cure Psoriasis Permanently: Is it Possible?
While there is currently no cure for psoriasis, ongoing research is being conducted to develop more effective treatments and potentially find a permanent solution. Treatment aims to manage symptoms, reduce inflammation, and improve quality of life.
It is essential to approach psoriasis treatment with realistic expectations. While it may not be possible to cure psoriasis permanently, with proper management and treatment, many individuals with psoriasis can lead fulfilling lives and keep their symptoms under control.
Related Articles
Connect With Us
Health In A Snap, Just One App.
KNOW MORE






























































































































































