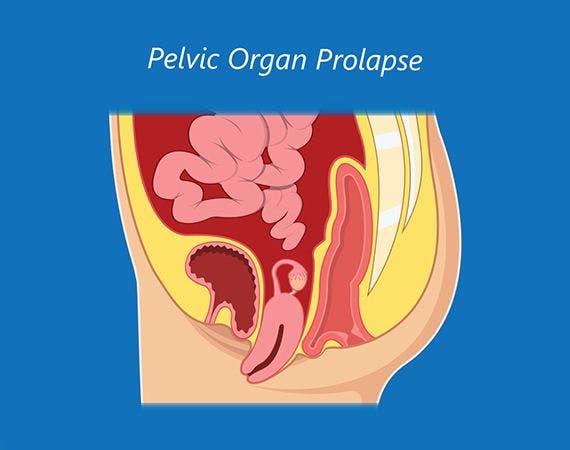
What is a Bladder Prolapse?
In women, the bladder is typically supported by a "hammock" of pelvic floor muscles and tissue. When these supportive structures are stretched or weakened, the bladder may descend and protrude into the vagina, a condition known as bladder prolapse or cystocele. Severe cases may lead to the prolapsed bladder appearing at the vaginal opening or even protruding through it. Bladder prolapse is a common issue among women, and while the symptoms can be bothersome, effective treatments are available.
Symptoms
The primary symptom of bladder prolapse is the sensation of a vaginal bulge, which can be observed or felt. Additional signs and symptoms associated with prolapse include:
1. Frequent voiding or a persistent urge to urinate.
2. Urinary incontinence characterized by the unintended loss of urine.
3. Lack of immediate relief after voiding.
4. Recurrent urinary tract infections.
5. Pain in the vagina, pelvis, lower abdomen, groin, or lower back.
6. The sensation of heaviness or pressure in the vaginal area.
7. Painful sexual intercourse.
8. Presence of tissue protruding from the vagina, which may be tender and/or bleeding.
It's important to note that some cases of prolapse may be asymptomatic.
Causes
Bladder prolapse can arise from various factors, with a primary cause being the strain placed on the supportive pelvic floor "hammock" during childbirth. Women who experience multiple pregnancies, deliver vaginally, or undergo prolonged or challenging childbirth are at an elevated risk.
Additional factors contributing to prolapse include:
1. Heavy lifting.
2. Chronic coughing or other respiratory issues.
3. Constipation.
4. Frequent straining during bowel movements.
5. Obesity.
6. Menopause, marked by a decline in oestrogen levels.
7. Previous pelvic surgery.
8. Aging.
These factors can weaken pelvic support structures, leading to bladder prolapse.
Treatment
Treatment Options for Bladder Prolapse:
- No treatment is required if the prolapse is not causing issues or blocking urine flow.
1. Conservative Management:
Behaviour Therapy: Includes Kegel exercises to strengthen pelvic floor muscles, pelvic floor physical therapy, and the use of a pessary (vaginal support device).
Drug Therapy: Involves oestrogen replacement therapy.
- Surgery aims to repair the body and alleviate symptoms, either through the vagina or abdomen.
- Various surgical approaches include open surgery (abdominal incision), minimally invasive surgery (small abdominal incisions), laparoscopic surgery (using abdominal wall incisions), and robot-assisted laparoscopic surgery (robotic instruments controlled by the surgeon).
- Surgical options include native tissue repair, augmentation with surgical material, and biological grafts.
- Before surgery, thorough discussions with the surgeon are crucial to understanding the risks, benefits, and choices. Informed consent is essential after all questions have been addressed.
2. Surgery:
If left untreated, bladder prolapse may remain stable or gradually worsen. In rare instances, severe prolapse can lead to kidney obstruction or urinary retention, potentially causing kidney damage or infection. Regular monitoring and timely intervention are essential for managing bladder prolapse effectively.
Speak to our team about Bladder Prolapse
Speak to our specialized team at Apex Hospitals to address any concerns or queries regarding Bladder Prolapse. Our experienced professionals are here to provide personalized guidance, discuss treatment options, and ensure your well-being. Your comfort and health are our top priorities. Don't hesitate to reach out and schedule a consultation. We are committed to delivering comprehensive, compassionate care tailored to your needs. Your journey to wellness starts with a conversation—contact us today.
FAQS
Health In A Snap, Just One App.
KNOW MORE